
Who we've helped
When a young person is told they have cancer, their world is turned upside down.
A world full of treatment, hospital visits and unexpected challenges.
One of these challenges is the financial impact of cancer on a family. At a time when the only worry parents should have is the health of their child, they are now deeply anxious and concerned about how to face the mounting bills. Parents can spend an average of £730 more every month when their child has cancer. This is made worse if a parent or carer has to leave work to look after their child. Costs such as travel to and from hospital, food and household bills, IT equipment, clothing, wigs and exercise equipment are just a few of the requests for financial help we receive on a daily basis.


Sophie’s story
Sophie was diagnosed with bowel cancer. She had multiple cycles of chemotherapy and immunotherapy treatments, extensive surgeries and radiotherapy. This has really limited Sophie in what she can do due to the physical recovery from her operations.


Adam’s Story
Adam came to us for support when he was 18 but back in 2008, Adam was diagnosed with a brain tumour – he was just four years old. He had 4 brain surgeries, but the tumour couldn’t be removed so he had 2 years of chemotherapy to try to stop it growing.
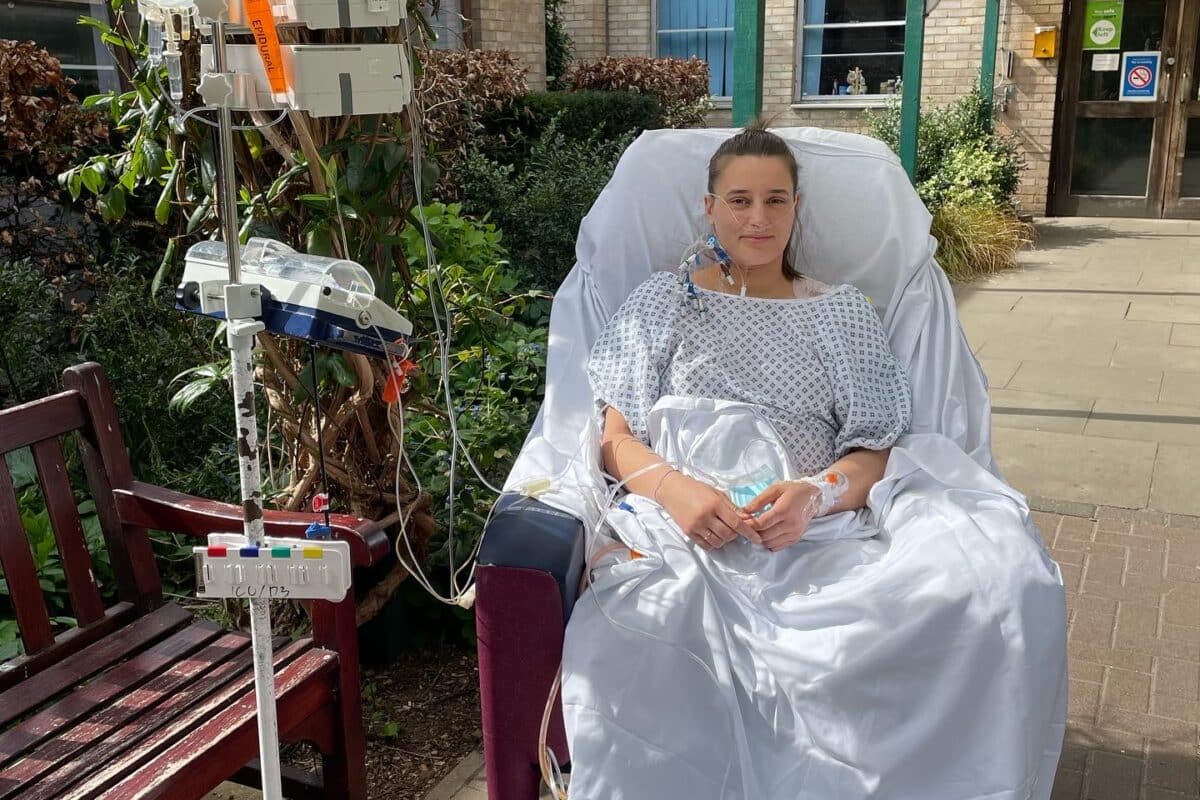

Emma’s Story
Emma is 21 and was studying forensic psychology at university. But in September 2021, the doctors found her first tumour. After many tests she finally had the devastating news that she had three malignant Paragangliomas. This is a neuroendocrine tumour.


Liam’s Story
Liam was 4 years old when he was first diagnosed with a form of brain tumour and underwent treatment. However, 12 years later a scan showed there had been disease progression. He started weekly chemotherapy, but a further scan showed that the tumour had not been responding to chemotherapy as hoped. This meant he would undergo complex surgery.


Premjeet’s Story
Premjeet was diagnosed with a brain tumour when he was 17. He wanted to re-sit his GCSE’s when feeling well enough, to enable him to start college the following September. Sadly, he didn’t have a laptop so couldn’t continue his studies.


Skye’s Story
My journey has definitely been a tough one, it took 10 months of misdiagnosing, 10 months of doctors and physios being adamant it was just sciatica. My tumour (osteosarcoma) had by then grown so big, it was the size of a grapefruit, pushing on my sciatic nerve.


Will’s Story
Will is 21 and was diagnosed with Acute lymphoblastic leukaemia in 2021. He had multiple lines of treatment, including a team cell transplant in late 2021. Unfortunately, Will relapsed.


Ezri’s Story
Hello again, my name is Ezri Payne, yes, I am named after a Star Trek character (thank you Dad), I am 18 years old and have just finished my final year of college (I think). My original plan was to finish college with flying colours and then study Paramedic Science at Anglia Ruskin. I love gruesome things, which is why I chose to have local anaesthetic to have my lump removed (yes it felt very strange 10/10 would NOT recommend) anyways I’ll get back to this. I think back to before my diagnosis and how lucky I was to be so blissfully unaware of the huge impact that one word can cause on someone. Now, I have had exposure to cancer when it sadly took the life of my grandparents, but I think it was hard for me to grasp the full extent of damage.
More families we have helped
Help us by donating today
A cancer diagnosis for anyone brings with it fear.
Fear of treatment, fear of tearing families apart, fear of money worries and fear of isolation. Please help take away the fear for these young people by donating today.